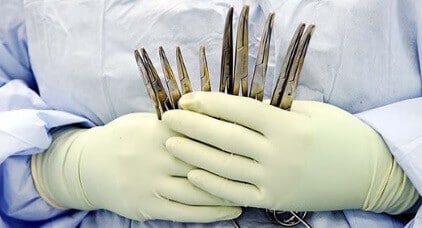
THOUSANDS of Australians are believed to be having unnecessary knee surgery despite evidence it could lead to life-threatening complications. Research published in The Medical Journal of Australia today found that while several studies over the past decade had concluded arthroscopies were ineffective for osteoarthritis of the knee, Victorian surgeons continued to use the procedure on
read more
The 37-year-old Yankee is now pitching like he did when he was a younger man, leading some to question whether banned substances, such as human growth hormone, were involved. Can injecting some stem cells into a damaged joint really help that much? Doctors extracted fat and bone marrow stem cells from baseball pitcher Bartolo Colon
read more
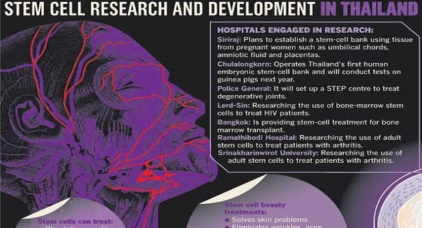
Thailand is fascinated with “roadmaps”, but when it comes to life-or-death matters like regenerative science, the country has none. Thai successes in stem-cell research have come despite a lack of funding or a national plan Thailand is fascinated with “roadmaps”, but when it comes to life-or-death matters like regenerative science, the country has none. Shinya
read more
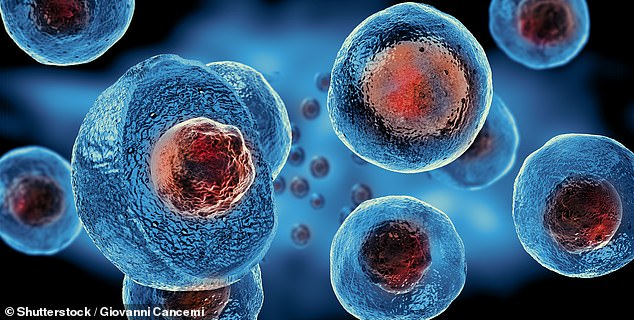
Miraculous stem cell revolution- Scientists hail breakthrough they claim is equal to the creation of anitbiotics to mend damaged hearts, heal strokes and cure blindness Stem cells were discovered by scientists in the 1960s in a major breakthrough The cells have enormous potential for the treatment of devastating conditions Scientists are working on techniques using
read more